Written by Khalil Al-Salem M.D
Cataract surgery in Jordan is a procedure to remove the lens of your eye and replace it with an artificial lens. In a healthy patient, the lens of your eye is clear. A cataract causes the lens to become cloudy, which eventually affects your vision. In this article, we will talk about types of cataract surgeries, complications of cataract surgery, and recovery tips after cataract surgery.
Cataract surgery is performed by a well-trained eye doctor (ophthalmologist) on an outpatient basis. This means no need to stay in the hospital once the operation ends. Cataract surgery in Jordan is considered the most second conventional surgery performed after Lasik surgery.

Why perform cataract surgery in Jordan?
Jordan is well known for it’s well equipped hospitals and well-trained personnels , Doctors master all types of cataract surgery, and we provide a quite variety of lenses to be implanted in the eye. patients who wish to get rid of the near glasses can be provided with lenses that has the ability to see near and far.
In addition, the complications of cataract surgery, at our hospital are minimal.
When to do cataract surgery ?
Cataract surgery is performed to treat lens opacities. Cataracts can cause blurry vision and increase the glare from lights. Suppose a cataract makes it difficult for you to carry out your normal activities. In that case, your doctor may urge you to do cataract surgery.
When a cataract interferes with the treatment of another eye problem, cataract surgery may be recommended. In rare cases, your doctor recommends cataract surgery if a cataract makes it difficult for your eye doctor to examine the back of your eye.
Some general health problems might affect the retina, which is capable of seeing the light. Diabetes and age-related macular degeneration might need close monitoring. This might force your doctor to push for cataract surgery.
In most cases, postponing cataract surgery won’t harm your eye, so you have time to consider your options. If your vision is still quite right, you may not need cataract surgery for many years.
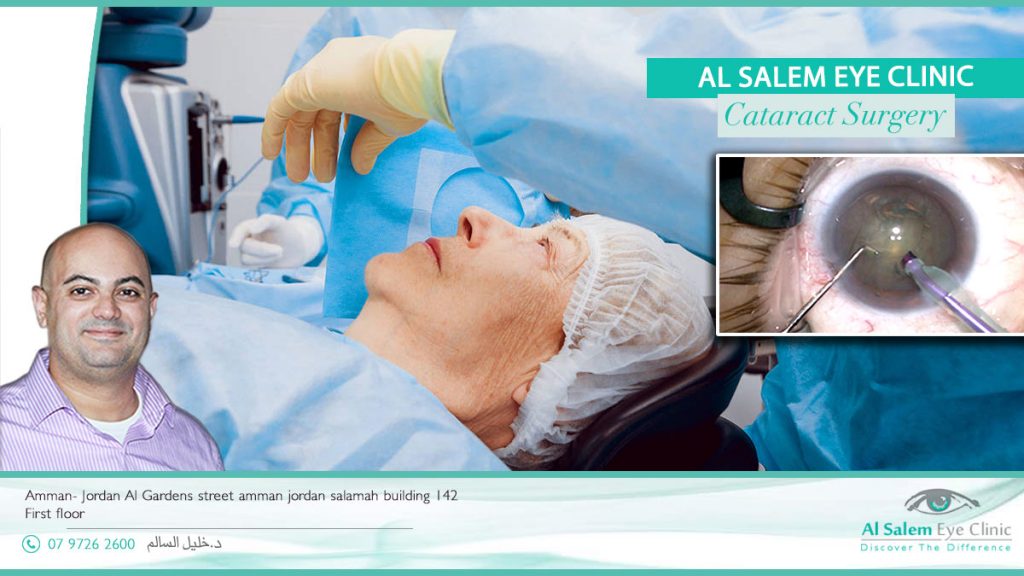
When considering cataract surgery, keep these questions in mind:
- Can you see to safely do your job and to drive?
- Do you have problems reading or watching television?
- Is it challenging to cook, shop, do yard work, climb stairs, or take medications?
- Do vision problems affect your level of independence?
- Do bright lights make it more challenging to see?
Complications of cataract surgery
Complications of cataract surgery are uncommon, and most can be treated successfully.
Cataract surgery risks include:
- Inflammation
- Infection
- Bleeding
- Swelling
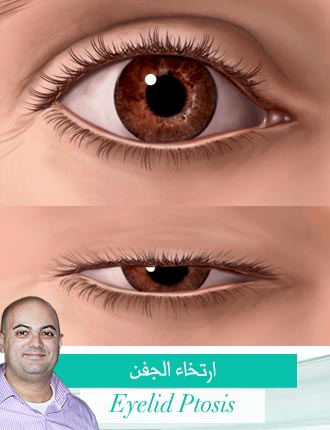
- Drooping eyelid
- Dislocation of artificial lens
- Retinal detachment
- Glaucoma
- Secondary cataract
- Loss of vision
Your risk of complications in cataract surgery is higher if you have another eye disease or a severe medical condition. Occasionally, the operation fails to improve vision because of underlying eye damage from other conditions, such as glaucoma or macular degeneration. It may be beneficial to evaluate and treat other eye problems before making the decision to have cataract surgery.
Recovery tips after cataract surgery , and how to prepare for it?
Food and medications
You may be instructed not to eat or drink anything 12 hours before cataract surgery. Your doctor may also advise you to temporarily stop taking any medication that could increase your bleeding risk during the procedure.
Let your doctor know if you take any medications for prostate problems. Some of these drugs can interfere with the operation .
It is essential to take your blood thinners before surgery, espcially for patients with heart problems.
Antibiotic eyedrops may be prescribed for use one or two days before the surgery.
Other precautions before cataract surgery
You can usually go home on the same day of surgery, but you won’t be able to drive, so arrange for a ride home.
It is advisable to arrange for help around the home, because your doctor may limit activities, such as bending and lifting up heavy objects a week after your surgery.
Patients are advised to pray while sitting as bending and kneeling is prohibited for a week after surgery.
Showering is allowed while closing the eye. No water or soup is allowed to enter the eye.
What you can expect after cataract surgery
Before the procedure
On the day of operation, your doctor performs a painless ultrasound test to measure your eye’s size and shape. This helps determine the right type of lens to be implanted.
Implanted lenses improve your vision by focusing light on the back of your eye. You won’t be able to see or feel the lens. It requires no care and becomes a permanent part of your eye.
A variety of lenses with different features are available. Ask Dr. Khalil Al-Salem for the best lens that will give you the most excellent comfort. Cost may also be a factor, as insurance companies may not pay for all types of lenses.
Types of lenses implanted in cataract surgery:
- Fixed-focus mono-focal. This type of lens has a single focus strength for distance vision. Reading will generally require the use of reading glasses. these are the most common types of lenses implanted in cataract surgery
- Accommodating-focus mono-focal. Although these lenses only have a single focusing strength, they can respond to eye muscle movements and shift focus to near or distant objects.
- Multifocal. These lenses are similar to glasses with bifocal or progressive lenses. Different areas of the lens have different focusing strengths, allowing for near, medium, and far vision.
- Astigmatism correction (toric). If you have significant astigmatism, a toric lens can help correct your vision.
Discuss the benefits and risks of the different types of IOLs with your eye surgeon to determine what’s best for you.
During the procedure
Cataract surgery is an outpatient procedure, which will take an hour or less to perform.
First, your doctor will place eyedrops in your eye to dilate your pupil. You’ll receive local anesthetics to numb the area, and you may be given a sedative to help you relax. If you’re given a sedative, you may remain awake, but groggy, during surgery.
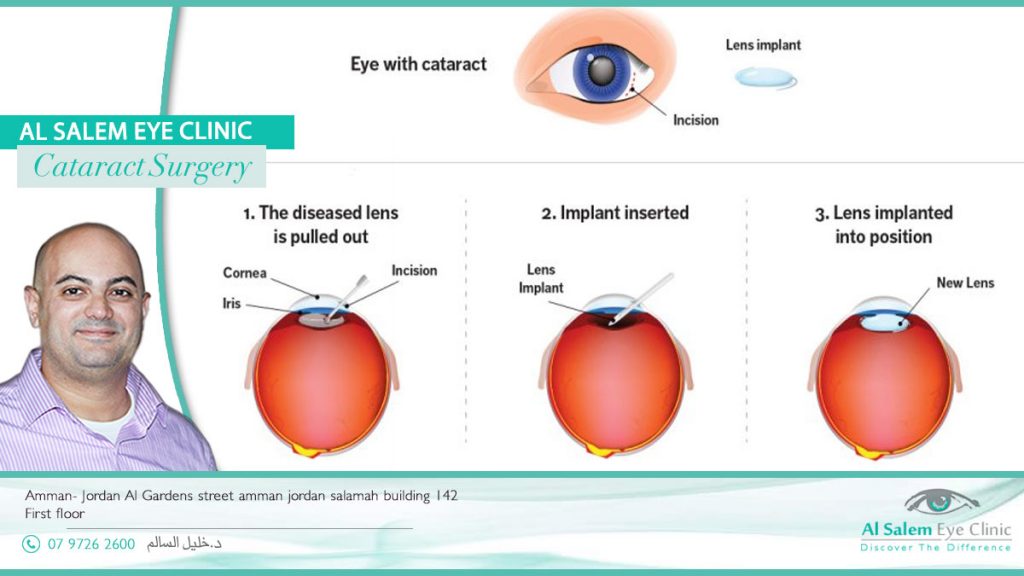
During cataract surgery, the clouded lens is removed, and a clear artificial lens is usually implanted. In some cases, however, a cataract may be removed without implanting a lens.
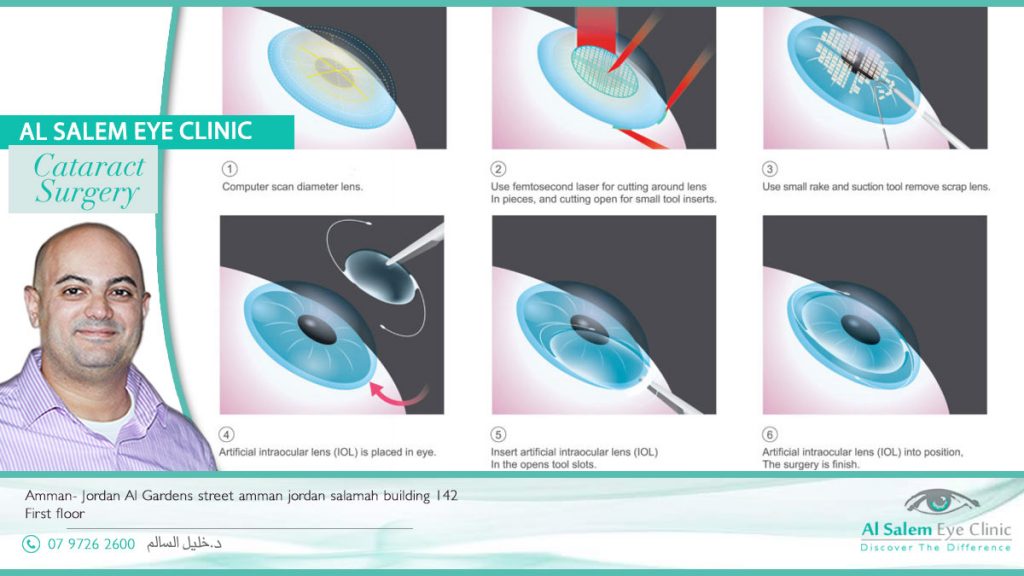
Surgical methods used to remove cataracts include:
- Using an ultrasound probe to break up the lens for removal. During a procedure called phacoemulsification.
Your surgeon makes a tiny incision in the front of your eye (cornea) and inserts a needle-thin probe into the lens substance where the cataract has formed.
- Your surgeon then uses the probe, which transmits ultrasound waves, to break up the cataract and suction the fragments. The very back of your lens (the lens capsule) is left intact to serve as a place for the artificial lens to rest. Stitches may be used to close the tiny incision in your cornea after the procedure.
- Making an incision in the eye and removing the lens in one piece. Extracapsular cataract extraction requires a larger incision than that used for phacoemulsification.
- Through this larger incision, your surgeon uses surgical tools to remove the lens’s front capsule and the cloudy lens comprising the cataract. The very posterior capsule of your lens is left in place to serve as a place for the artificial lens to rest.
- This procedure may be performed if you have certain eye complications. With the larger incision, stitches are required.
Once the cataract has been removed by either phacoemulsification or extracapsular extraction, the artificial lens is implanted into the empty lens capsule.
Recovery tips after cataract surgery
After the operation, expect your vision to begin improving within a few days. Your vision may be blurry at first as your eye heals and adjusts.
Colors may seem brighter after your surgery because you are looking through a new, clear lens. a lens opacity is usually yellow- or brown-tinted before surgery, muting the look of colors.
You’ll usually see your eye doctor a day or two after your surgery, the following week, and then again after about a month to monitor healing.
It’s normal to feel itching and mild discomfort for a couple of days after surgery. Avoid rubbing or pushing on your eye.
Your doctor may ask you to wear an eye patch or protective shield on the day of surgery. Your doctor may also recommend wearing the eye patch a few days after your surgery and the protective shield when you sleep during the recovery period.
Your doctor may prescribe eye drops or other medication to prevent infection, reduce inflammation, and control eye pressure. Sometimes, these medications can be injected into the eye at the time of surgery.
After a couple of days, most of the discomfort should disappear. Often, complete healing occurs within eight weeks.
Contact your doctor immediately if you experience any of the following:
- Vision loss
- Pain that persists despite the use of over-the-counter pain medications
- Increased eye redness
- Eyelid swelling
- Light flashes or multiple new spots (floaters) in front of your eye
Most people need glasses, at least some of the time, after cataract surgery. Your doctor will let you know when your eyes have healed enough to get a final prescription for eyeglasses. This is usually between one and three months after surgery.
If you have cataracts in both eyes, your doctor usually schedules the second surgery after the first eye has healed.
Results
Cataract surgery successfully restores vision in the majority of people who have the procedure.
People who’ve had cataract surgery may develop a secondary lens opacity. The medical term for this common complication is known as posterior capsule opacification (PCO).
PCO is treated with a painless, five-minute outpatient procedure called yttrium-aluminum-garnet (YAG) laser capsulotomy. In YAG laser capsulotomy, a laser beam is used to make a small opening in the clouded capsule to provide a clear path through which the light can pass.
After the procedure, you usually stay in the doctor’s office for about an hour to make sure your eye pressure doesn’t rise. Other complications are rare but can include increased eye pressure and retinal detachment.

 تخطي إلى المحتوى
تخطي إلى المحتوى