Written by: Prof. Khalil Al-Salem
Anisocoria, or unequal pupils, is a common clinical finding that may be benign or clinically significant. It can be related to physiological variation, but it may also indicate conditions such as Horner syndrome or Adie’s pupil. In addition, medication causing mydriasis should always be considered, as it is a frequent and often overlooked cause. Therefore, understanding the causes of anisocoria and recognizing when unequal pupils require urgent evaluation is essential in daily clinical practice.
What is Anisocoria ?
Anisocoria refers to a difference in pupil size between the two eyes. It is frequently encountered in clinical settings. In many individuals, this difference is harmless. However, in some cases, it may reflect underlying pathology. Therefore, a careful and structured approach is required when evaluating unequal pupils.
The first step is to confirm that anisocoria is truly present. A small difference, usually less than 1 mm, can be normal. This is known as physiological anisocoria. It is relatively common and can be seen in a significant portion of the population. Importantly, the degree of anisocoria remains similar in both light and dark conditions. In addition, patients typically do not have any associated symptoms.
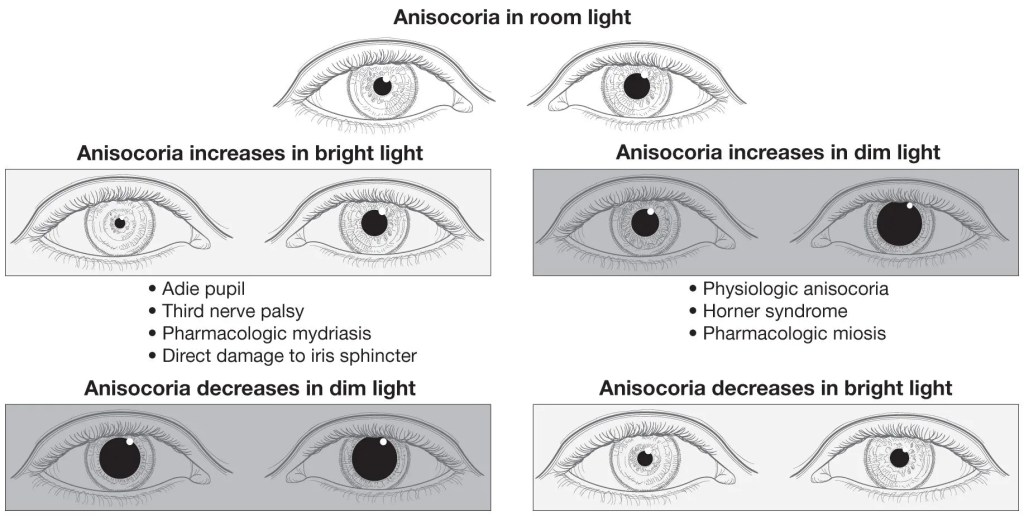
However, when the difference in pupil size changes with lighting conditions, the situation becomes more important. This helps identify which pupil is abnormal. If anisocoria increases in the dark, the smaller pupil is abnormal. In contrast, if anisocoria increases in bright light, the larger pupil is the abnormal one. This simple observation provides a strong clinical clue.
When the smaller pupil is abnormal, sympathetic pathway dysfunction should be suspected. Horner syndrome is the most important condition in this group. It is characterized by mild ptosis, miosis, and sometimes anhidrosis. Although these features may be subtle, they are clinically significant. In addition, the affected pupil may show dilation lag when the lights are turned off.
The most common causes of Anisocoria
The causes of Horner syndrome can vary widely. Some are benign, while others are serious. For example, it may result from trauma or previous surgery. However, it can also be associated with carotid artery dissection or tumors. Therefore, once suspected, further evaluation is necessary. Imaging studies are often required to rule out life-threatening conditions.
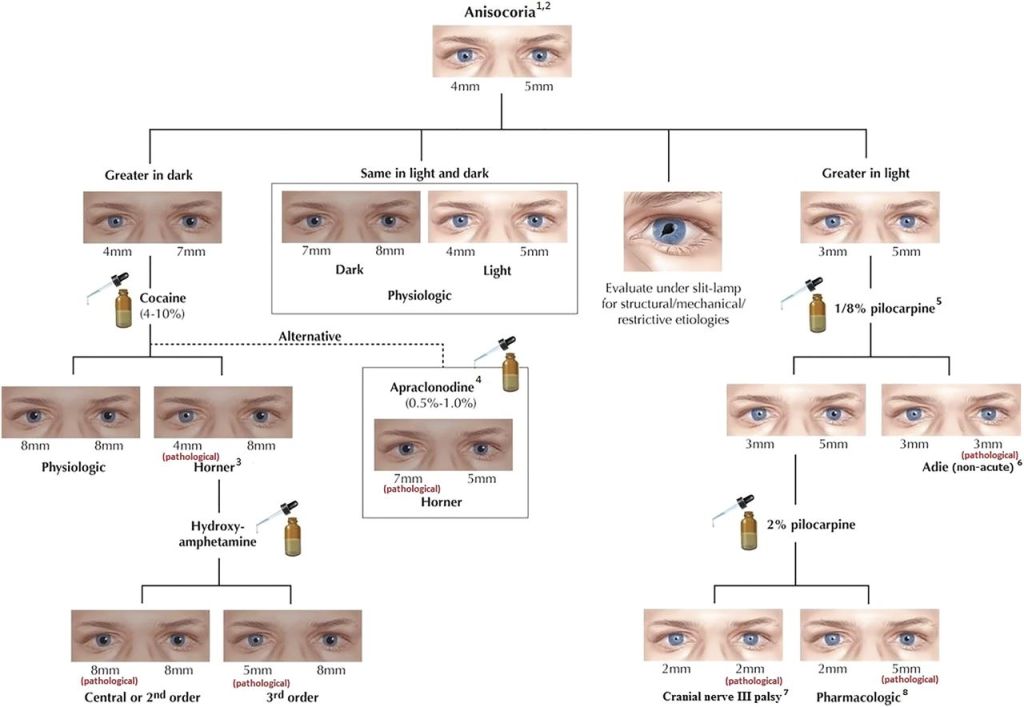
On the other hand, when the larger pupil is abnormal, parasympathetic dysfunction should be considered. One common example is Adie’s pupil. This condition typically affects young adults. The pupil appears dilated and reacts poorly to light. However, it constricts better during near vision. This phenomenon is known as light-near dissociation.
Adie’s pupil is usually benign. Nevertheless, it may cause visual discomfort. Patients often complain of glare or difficulty focusing. Over time, the affected pupil may become smaller. Although it is not dangerous, it is important to recognize it correctly to avoid unnecessary concern.
Medication trauma and Mydriasis
Medication causing mydriasis is another important cause of anisocoria. This is often overlooked in clinical practice. Many medications can affect pupil size. For instance, anticholinergic drugs such as atropine can lead to dilation. In addition, exposure to certain inhalers or eye drops may produce similar findings.
In many cases, medication-induced anisocoria is unilateral. This can happen when one eye is accidentally exposed to the drug. The affected pupil is usually dilated and poorly reactive. However, there are no associated neurological signs. Therefore, taking a careful history is extremely important in these situations.
Despite these relatively benign causes, more serious conditions must always be considered. Third nerve palsy is one of them. It may present with a dilated pupil, ptosis, and limitation of eye movements. Patients may also report double vision. This condition requires urgent assessment, as it may be caused by an aneurysm.
Trauma is another possible explanation for unequal pupils. Direct injury to the iris can lead to structural abnormalities. As a result, the pupil may appear irregular or fixed. Surgical procedures involving the eye can also produce similar changes. Therefore, previous trauma or surgery should always be explored.
Although many cases of anisocoria are harmless, certain warning signs should not be ignored. Sudden onset is always concerning. In addition, associated symptoms such as headache, eye pain, or neurological deficits increase the level of suspicion. In these situations, urgent referral is necessary.
Clinical Examination in Anisocoria
Clinical examination remains the cornerstone of diagnosis. Pupils should be evaluated in both bright and dim light. Their size, shape, and reactivity should be carefully assessed. In addition, eyelid position and eye movements should be examined. This helps in identifying associated neurological signs.
Pharmacological testing can be helpful in selected cases. For example, dilute pilocarpine may confirm Adie’s pupil. Similarly, apraclonidine can support the diagnosis of Horner syndrome. However, these tests should be used selectively. Clinical judgment is still the most important factor.
In conclusion, anisocoria is a common but important finding. While many cases are benign, some may indicate serious disease. Therefore, understanding the behavior of unequal pupils in different lighting conditions is essential. In addition, recognizing key causes such as Horner syndrome, Adie’s pupil, and medication causing mydriasis allows for accurate diagnosis. A careful history and thorough examination remain the most reliable tools in clinical practice.
 تخطي إلى المحتوى
تخطي إلى المحتوى