بقلم أ.د. خليل السالم ، إلقاء و تحضير د. الاء خميس
Neuromyelitis Optica Spectrum Disorders (NMOSD) are rare autoimmune inflammatory diseases of the central nervous system that predominantly affect the optic nerves, spinal cord, and selected brain regions. Neuromyelitis optica was historically misclassified as a form of multiple sclerosis; however, NMOSD is now clearly recognized as a separate disease entity with distinct immunological mechanisms, imaging features, and therapeutic requirements. Early recognition of NMOSD is critical, as delayed diagnosis may result in irreversible neurological disability.
Autoimmune Pathophysiology of NMOSD
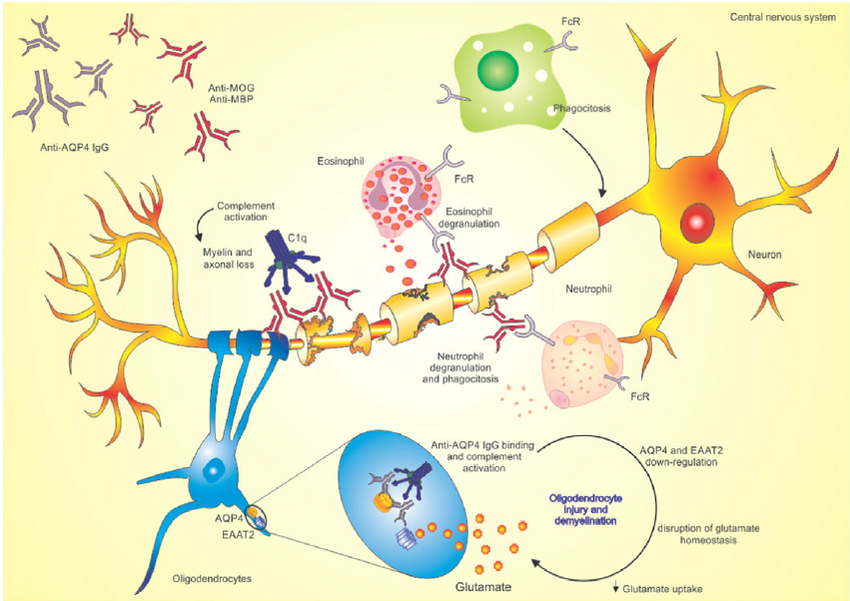
The pathogenesis of neuromyelitis optica spectrum disorders is driven by an autoimmune response against astrocytes rather than primary demyelination. Most patients with NMOSD harbor pathogenic immunoglobulin G antibodies directed against aquaporin-4 (AQP4), a water channel protein expressed on astrocytic foot processes at the blood–brain barrier. Binding of aquaporin-4 antibodies activates complement-mediated cytotoxicity, leading to astrocyte destruction, secondary demyelination, and neuronal injury. This astrocytopathy explains why NMOSD attacks are often severe, necrotizing, and associated with poor spontaneous recovery when compared to multiple sclerosis.
Clinical Presentation and NMOSD Symptoms
Neuromyelitis optica spectrum disorders typically present with relapsing episodes of optic neuritis, longitudinally extensive transverse myelitis, or area postrema syndrome. Optic neuritis in NMOSD is frequently bilateral or recurrent and may result in profound and permanent visual loss. Spinal cord involvement is characterized by inflammation extending across three or more vertebral segments, leading to acute weakness, sensory loss, and bladder or bowel dysfunction. Area postrema syndrome is a highly specific manifestation of NMOSD and presents with persistent hiccups, nausea, and vomiting due to medullary involvement. Brain manifestations may also occur, particularly in aquaporin-4–rich regions such as the hypothalamus and periventricular areas.
Diagnosis of Neuromyelitis Optica Spectrum Disorders
The diagnosis of neuromyelitis optica spectrum disorders relies on clinical criteria, antibody testing, and magnetic resonance imaging findings. Detection of serum aquaporin-4 immunoglobulin G antibodies using cell-based assays is highly specific for NMOSD and confirms the diagnosis in most patients. A smaller subgroup of patients may test negative for aquaporin-4 antibodies but have antibodies against myelin oligodendrocyte glycoprotein, indicating a related but distinct disease phenotype. MRI typically reveals longitudinally extensive spinal cord lesions, optic nerve inflammation, and characteristic brain lesions that help differentiate NMOSD from multiple sclerosis.
Acute Treatment of NMOSD Attacks
Acute relapses of neuromyelitis optica spectrum disorders constitute neurological emergencies that require immediate treatment. High-dose intravenous corticosteroids are the first-line therapy and aim to suppress active immune-mediated inflammation. In patients who fail to respond adequately, plasma exchange is strongly recommended and has proven efficacy in removing circulating pathogenic antibodies. Early intervention during acute NMOSD attacks significantly improves functional recovery and reduces long-term disability.
Long-Term Management and Relapse Prevention
Long-term treatment of neuromyelitis optica spectrum disorders focuses on preventing relapses, as cumulative disability in NMOSD is relapse-dependent rather than progressive. Conventional immunosuppressive therapies such as azathioprine, mycophenolate mofetil, and B-cell–depleting agents have been widely used to reduce relapse frequency. In recent years, targeted biologic therapies specifically developed for NMOSD have transformed disease management by inhibiting complement activation, interleukin-6 signaling, or antibody-producing B cells. These therapies offer improved disease control with greater specificity and reduced relapse risk.
Prognosis and Long-Term Outcomes
The prognosis of neuromyelitis optica spectrum disorders has improved substantially with early diagnosis and modern immunotherapy. Nevertheless, untreated or misdiagnosed NMOSD may result in severe visual impairment, paraplegia, chronic pain, and reduced quality of life. Long-term care requires regular monitoring, adherence to therapy, and a multidisciplinary approach involving neurologists, ophthalmologists, and rehabilitation specialists to optimize functional outcomes.
Conclusion
Neuromyelitis Optica Spectrum Disorders are distinct autoimmune diseases characterized by aquaporin-4 antibody–mediated astrocyte injury, severe inflammatory attacks, and relapse-driven disability. Advances in diagnostic testing and targeted treatment have dramatically improved outcomes for patients with NMOSD. Early recognition, accurate diagnosis, and sustained immunotherapy remain the cornerstones of effective neuromyelitis optica spectrum disorder management.
 تخطي إلى المحتوى
تخطي إلى المحتوى
